
- •Contents
- •Foreword
- •1.1.1 Haemostasis
- •1.1.2 Inflammatory Phase
- •1.1.3 Proliferative Phase
- •1.1.4 Remodelling and Resolution
- •1.7 The Surgeon’s Preoperative Checklist
- •1.8 Operative Note
- •2.4.1 Local Risks
- •2.4.2 Systemic Risks
- •2.5 Basic Oral Anaesthesia Techniques
- •2.5.1 Buccal Infiltration Anaesthetic
- •2.5.2 Mandibular Teeth
- •2.5.2.1 Conventional ‘Open-Mouth’ Technique
- •2.5.2.2 Akinosi ‘Closed-Mouth’ Technique
- •2.5.2.3 Gow–Gates Technique
- •2.5.2.4 Mandibular Long Buccal Block
- •2.5.2.5 Mental Nerve Block
- •2.5.3 Maxillary Teeth
- •2.5.3.1 Greater Palatine Block
- •2.5.3.2 Palatal Infiltration
- •2.5.3.3 Nasopalatine Nerve Block
- •2.5.3.4 Posterior Superior Alveolar Nerve Block
- •2.6 Adjunct Methods of Local Anaesthesia
- •2.6.1 Intraligamentary Injection
- •2.6.2 Intrapulpal Injection
- •2.7 Troubleshooting
- •3.1 Retractors
- •3.2 Elevators, Luxators, and Periotomes
- •3.3 Dental Extraction Forceps
- •3.4 Ancillary Soft Tissue Instruments
- •3.5 Suturing Instruments
- •3.6 Surgical Suction
- •3.7 Surgical Handpiece and Bur
- •3.8 Surgical Irrigation Systems
- •3.9 Mouth Props
- •4.1 Maxillary Incisors
- •4.2 Maxillary Canines
- •4.3 Maxillary Premolars
- •4.4 Maxillary First and Second Molars
- •4.5 Mandibular Incisors
- •4.6 Mandibular Canines and Premolars
- •4.7 Mandibular Molars
- •5.3 Common Soft Tissue Flaps for Dental Extraction
- •5.4 Bone Removal
- •5.5 Tooth Sectioning
- •5.6 Cleanup and Closure
- •6.2 Damage to Adjacent Teeth or Restorations
- •7.4.1.1 Erupted
- •7.4.1.2 Unerupted/Partially Erupted
- •7.4.2 Mandibular Third Molars
- •7.4.2.1 Mesioangular
- •7.4.2.2 Distoangular/Vertical
- •7.4.2.3 Horizontal
- •7.4.2.4 Full Bony Impaction (Early Root Development)
- •8.1 Ischaemic Cardiovascular Disease
- •8.5 Diabetes Mellitus
- •8.6.1 Bleeding Diatheses
- •8.6.2 Medications
- •8.6.2.1 Management of Antiplatelet Agents Prior to Dentoalveolar Surgery
- •8.6.2.2 Management of Patients Taking Warfarin Prior to Dentoalveolar Surgery
- •8.6.2.3 Management of Patients Taking Direct Anticoagulant Agents Prior to Dentoalveolar Surgery
- •8.8 The Irradiated Patient
- •8.8.1 Management of the Patient with a History of Head and Neck Radiotherapy
- •9.5.1 Alveolar Osteitis
- •9.5.2 Acute Facial Abscess
- •9.5.3 Postoperative Haemorrhage
- •9.5.4 Temporomandibular Joint Disorder
- •9.5.5 Epulis Granulomatosa
- •9.5.6 Nerve Injury
- •B.1.3 Consent
- •B.1.4 Local Anaesthetic
- •B.1.5 Use of Sedation
- •B.1.6 Extraction Technique
- •B.1.7 Outcomes Following Extraction
- •B.2.1 Deciduous Incisors and Canines
- •B.2.2 Deciduous Molars
- •Bibliography
- •Index
30 2 Local Anaesthesia
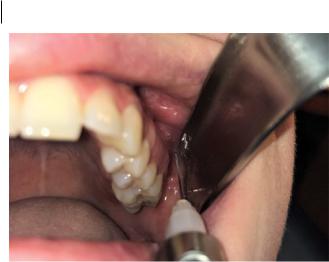
Figure 2.14 Posterior superior alveolar nerve block.
4)Insert the needle into the vestibular mucosa just posterior to the maxillary tuberosity, angled at 45° to the occlusal plane (Figure 2.14). Advance it approximately 1–1.5 cm.
5)Aspirate the syringe to ensure the needle point has not traversed the intravascular space of a blood vessel.
6)Deposit the anaesthetic solution slowly; a slow rate of injection significantly reduces discomfort for the patient.
7)Allow the local anaesthetic sufficient time to anaesthetise the tissues, based upon the pharmacokinetic properties of the solution, and monitor the patient for any adverse reaction.
2.6 Adjunct Methods of Local Anaesthesia
In certain situations of dental extraction, it may be difficult to obtain complete anaesthesia using the standard infiltration and block techniques described in the previous section. The following methods may be utilised if additional anaesthesia of a single tooth is required mid-procedure. Note that they cannot be used alone to obtain sufficient anaesthesia for dental extraction.
2.6.1 Intraligamentary Injection
1)Advance a short needle into the periodontal ligament space. The needle should be felt to ‘wedge’ into the space between tooth and bone; this is required to ensure the anaesthetic solution is delivered into the correct site.
2)Deposit the anaesthesia. Firm pressure on the syringe will be required to deposit the solution. Due to the extremely small periodontal ligament space, only minute volumes of solution can be injected using this technique.
3)Repeat in at least four positions around the tooth.
4)Allow the local anaesthetic sufficient time to anaesthetise the tissues, based upon the pharmacokinetic properties of the solution, and monitor the patient for any adverse reaction.
https://t.me/DentalBooksWorld
2.6 Adjunct MctthAds hof hncal ucMdscttMdssc |
31 |
|
|
2.6.2Intrapulpal Injection
Intrapulpal injection is useful in cases where an attempt to section a tooth has already been made and the patient has experienced pain during instrumenting or sectioning. As the name suggests, the anaesthetic agent is injected into the pulp chamber to directly anaesthetise the pulpal tissues.
1)Position the patient in the dental chair, allowing for adequate light and access to the dental pulp.
2)Visualise the pulp chamber – this will be the site of needle entry.
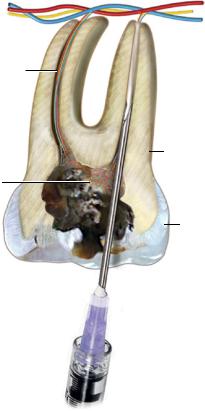
3)Advance a short needle into the pulp chamber (Figure 2.15).
4)Deposit local anaesthetic into the pulp. As the volume of the pulp chamber is small, only a minute volume of anaesthetic is required to achieve pulpal anaesthesia. It may be necessary to apply firm pressure on the syringe in order to deliver the solution into the chamber.
5)Allow the local anaesthetic sufficient time to anaesthetise the tissues, based upon the pharmacokinetic properties of the solution, and monitor the patient for any adverse reaction.
Middle superior alveolar neurovascular bundle
Root canal |
|
Injection of |
|
|
|
|
|
anaesthetic |
|
|
|
|
|
agent |
Dentine
Chamber pulp
Decay |
Enamel |
|
Figure 2.15 Intrapulpal injection.
https://t.me/DentalBooksWorld
