
- •ICU Protocols
- •Preface
- •Acknowledgments
- •Contents
- •Contributors
- •1: Airway Management
- •Suggested Reading
- •2: Acute Respiratory Failure
- •Suggested Reading
- •Suggested Reading
- •Website
- •4: Basic Mechanical Ventilation
- •Suggested Reading
- •Suggested Reading
- •Websites
- •Suggested Reading
- •Websites
- •7: Weaning
- •Suggested Reading
- •8: Massive Hemoptysis
- •Suggested Reading
- •9: Pulmonary Thromboembolism
- •Suggested Reading
- •Suggested Reading
- •Websites
- •11: Ventilator-Associated Pneumonia
- •Suggested Readings
- •12: Pleural Diseases
- •Suggested Reading
- •Websites
- •13: Sleep-Disordered Breathing
- •Suggested Reading
- •Websites
- •14: Oxygen Therapy
- •Suggested Reading
- •15: Pulse Oximetry and Capnography
- •Conclusion
- •Suggested Reading
- •Websites
- •16: Hemodynamic Monitoring
- •Suggested Reading
- •Websites
- •17: Echocardiography
- •Suggested Readings
- •Websites
- •Suggested Reading
- •Websites
- •19: Cardiorespiratory Arrest
- •Suggested Reading
- •Websites
- •20: Cardiogenic Shock
- •Suggested Reading
- •21: Acute Heart Failure
- •Suggested Reading
- •22: Cardiac Arrhythmias
- •Suggested Reading
- •Website
- •23: Acute Coronary Syndromes
- •Suggested Reading
- •Website
- •Suggested Reading
- •25: Aortic Dissection
- •Suggested Reading
- •26: Cerebrovascular Accident
- •Suggested Reading
- •Websites
- •27: Subarachnoid Hemorrhage
- •Suggested Reading
- •Websites
- •28: Status Epilepticus
- •Suggested Reading
- •29: Acute Flaccid Paralysis
- •Suggested Readings
- •30: Coma
- •Suggested Reading
- •Suggested Reading
- •Websites
- •32: Acute Febrile Encephalopathy
- •Suggested Reading
- •33: Sedation and Analgesia
- •Suggested Reading
- •Websites
- •34: Brain Death
- •Suggested Reading
- •Websites
- •35: Upper Gastrointestinal Bleeding
- •Suggested Reading
- •36: Lower Gastrointestinal Bleeding
- •Suggested Reading
- •37: Acute Diarrhea
- •Suggested Reading
- •38: Acute Abdominal Distension
- •Suggested Reading
- •39: Intra-abdominal Hypertension
- •Suggested Reading
- •Website
- •40: Acute Pancreatitis
- •Suggested Reading
- •Website
- •41: Acute Liver Failure
- •Suggested Reading
- •Suggested Reading
- •Websites
- •43: Nutrition Support
- •Suggested Reading
- •44: Acute Renal Failure
- •Suggested Reading
- •Websites
- •45: Renal Replacement Therapy
- •Suggested Reading
- •Website
- •46: Managing a Patient on Dialysis
- •Suggested Reading
- •Websites
- •47: Drug Dosing
- •Suggested Reading
- •Websites
- •48: General Measures of Infection Control
- •Suggested Reading
- •Websites
- •49: Antibiotic Stewardship
- •Suggested Reading
- •Website
- •50: Septic Shock
- •Suggested Reading
- •51: Severe Tropical Infections
- •Suggested Reading
- •Websites
- •52: New-Onset Fever
- •Suggested Reading
- •Websites
- •53: Fungal Infections
- •Suggested Reading
- •Suggested Reading
- •Website
- •55: Hyponatremia
- •Suggested Reading
- •56: Hypernatremia
- •Suggested Reading
- •57: Hypokalemia and Hyperkalemia
- •57.1 Hyperkalemia
- •Suggested Reading
- •Website
- •58: Arterial Blood Gases
- •Suggested Reading
- •Websites
- •59: Diabetic Emergencies
- •59.1 Hyperglycemic Emergencies
- •59.2 Hypoglycemia
- •Suggested Reading
- •60: Glycemic Control in the ICU
- •Suggested Reading
- •61: Transfusion Practices and Complications
- •Suggested Reading
- •Websites
- •Suggested Reading
- •Website
- •63: Onco-emergencies
- •63.1 Hypercalcemia
- •63.2 ECG Changes in Hypercalcemia
- •63.3 Superior Vena Cava Syndrome
- •63.4 Malignant Spinal Cord Compression
- •Suggested Reading
- •64: General Management of Trauma
- •Suggested Reading
- •65: Severe Head and Spinal Cord Injury
- •Suggested Reading
- •Websites
- •66: Torso Trauma
- •Suggested Reading
- •Websites
- •67: Burn Management
- •Suggested Reading
- •68: General Poisoning Management
- •Suggested Reading
- •69: Syndromic Approach to Poisoning
- •Suggested Reading
- •Websites
- •70: Drug Abuse
- •Suggested Reading
- •71: Snakebite
- •Suggested Reading
- •72: Heat Stroke and Hypothermia
- •72.1 Heat Stroke
- •72.2 Hypothermia
- •Suggested Reading
- •73: Jaundice in Pregnancy
- •Suggested Reading
- •Suggested Reading
- •75: Severe Preeclampsia
- •Suggested Reading
- •76: General Issues in Perioperative Care
- •Suggested Reading
- •Web Site
- •77.1 Cardiac Surgery
- •77.2 Thoracic Surgery
- •77.3 Neurosurgery
- •Suggested Reading
- •78: Initial Assessment and Resuscitation
- •Suggested Reading
- •79: Comprehensive ICU Care
- •Suggested Reading
- •Website
- •80: Quality Control
- •Suggested Reading
- •Websites
- •81: Ethical Principles in End-of-Life Care
- •Suggested Reading
- •82: ICU Organization and Training
- •Suggested Reading
- •Website
- •83: Transportation of Critically Ill Patients
- •83.1 Intrahospital Transport
- •83.2 Interhospital Transport
- •Suggested Reading
- •84: Scoring Systems
- •Suggested Reading
- •Websites
- •85: Mechanical Ventilation
- •Suggested Reading
- •86: Acute Severe Asthma
- •Suggested Reading
- •87: Status Epilepticus
- •Suggested Reading
- •88: Severe Sepsis and Septic Shock
- •Suggested Reading
- •89: Acute Intracranial Hypertension
- •Suggested Reading
- •90: Multiorgan Failure
- •90.1 Concurrent Management of Hepatic Dysfunction
- •Suggested Readings
- •91: Central Line Placement
- •Suggested Reading
- •92: Arterial Catheterization
- •Suggested Reading
- •93: Pulmonary Artery Catheterization
- •Suggested Reading
- •Website
- •Suggested Reading
- •95: Temporary Pacemaker Insertion
- •Suggested Reading
- •96: Percutaneous Tracheostomy
- •Suggested Reading
- •97: Thoracentesis
- •Suggested Reading
- •98: Chest Tube Placement
- •Suggested Reading
- •99: Pericardiocentesis
- •Suggested Reading
- •100: Lumbar Puncture
- •Suggested Reading
- •Website
- •101: Intra-aortic Balloon Pump
- •Suggested Reading
- •Appendices
- •Appendix A
- •Appendix B
- •Common ICU Formulae
- •Appendix C
- •Appendix D: Syllabus for ICU Training
- •Index

Lumbar Puncture |
100 |
|
|
Rajesh Chawla and Charu Gauba |
|
A 40-year-old male patient was admitted to hospital with altered sensorium, headache, vomiting, high-grade fever and rash. He was drowsy. His pulse was 120/min and blood pressure was 110/80 mmHg. Neck rigidity was positive and CT scan report of the head was normal. A lumbar puncture (LP) was planned.
Lumbar puncture is a commonly performed procedure to obtain cerebrospinal fluid (CSF) for diagnosis of various neurological disorders.
Step 1: Assess the need for lumbar puncture
A.Diagnostic indications
•Infectious disease
–Meningitis
•Tubercular
•Viral
•Bacterial
•Fungal
–Encephalitis
•Subarachnoid hemorrhage (SAH)
•Demyelinating/inflammatory diseases
–Multiple sclerosis/acute disseminated encephalomyelitis
–Guillain–Barré syndrome/chronic inflammatory demyelinating polyneuropathy
–Neurosarcoid
R. Chawla, M.D., F.C.C.M. (*)
Department of Respiratory, Critical Care & Sleep Medicine, Indraprastha Apollo Hospitals, New Delhi, India
e-mail: drchawla@hotmail.com
C. Gauba, M.D., D.N.B.
Department of Neurology, Indraprastha Apollo Hospitals, New Delhi, India
R. Chawla and S. Todi (eds.), ICU Protocols: A stepwise approach, |
805 |
DOI 10.1007/978-81-322-0535-7_100, © Springer India 2012 |
|
806 |
R. Chawla and C. Gauba |
|
|
•Neurodiagnostic imaging
–Myelography
–Cisternography
•CSF pressure (opening pressure)
–Normal pressure hydrocephalus (NPH)
–Idiopathic intracranial hypertension (IIH)
•Oncologic procedures
•Carcinomatous meningitis
•Central nervous system lymphoma B. Therapeutic indications
•Neuraxial analgesia and anesthesia
–Narcotics
–Local anesthetics
•Ventriculitis and post-instrumentation meningitis
–Antibiotic administration
•Leukemias and lymphomas with cerebrospinal involvement
–Chemotherapy
–Methotrexate
•Draining CSF in NPH and IIH
Step 2: Be familiar with the CSF analysis
Tests on CSF are determined by:
•Age
•Clinical history
•Differential diagnosis Basic investigations
•Biochemical
–Glucose
•Approximately two-third of serum glucose or higher.
•Decreased levels below 40–50% of serum glucose generally imply a bacterial infection.
•Simultaneously random blood sugar must be checked.
–Protein (<0.5% of plasma)
•CSF total protein: 15–45 mg/100 mL
•Approximately 1,000 RBCs = 1 mg% protein (in a bloody tap)
•Increased protein
–Infective and post-infective state
–Demyelinating polyneuropathies
•Hematology
–Cell counts
•Total
–Maximum 5 WBCs/mL; RBCs nil
–In bloody tap 1, WBC per approximately 700 RBCs can exist
•Differential
100 Lumbar Puncture |
807 |
|
|
•Microbiology
–Stains: gram/fungal/acid fast/India ink
–Cultures: aerobic/fungal/tubercular
•Immunology
–Cryptococcal antigen
–Bacterial antigens
–Viral (e.g., herpes simplex PCR)
–Mycobacterial (TB PCR)
–Immunoglobulins
–Oligoclonal band
–Cysticercus antibody
–VDRL
•Cytology
–Malignancies
Step 3: Rule out the contraindications
A.Absolute
•Infected skin over the needle entry site
•Risk/signs of cerebral herniation
–Intracranial lesions especially posterior fossa tumors
–Intraspinal mass, especially intramedullary
–Focal neurological signs
–Brain stem signs
•Pupillary changes
•Decerebrate posturing
•Altered respiration
B.Relative
•Raised intracranial pressure (ICP)
•Cardiorespiratory compromise: position related
•Coagulopathy/thrombocytopenia (platelet count <50,000 or INR >1.5): risk of spinal hematoma
•Previous lumbar surgery/congenital defects/degeneration: may require radiology guidance
Step 4: Order CT head before lumbar puncture
•In all patients to rule out mass effect/frank bleeding, especially if there is:
–Age > 60 years
–Immunocompromised patient with known CNS lesions
–Altered sensorium
–Focal neurological deficit
–Seizure within past 1 week
–Papilledema
–Suspicion of raised ICP
CT does not always rule out the risk of herniation completely.
808 |
R. Chawla and C. Gauba |
|
|
Step 5: Informed consent
•Discuss the prognosis of the patient and the need for the procedure.
•Explain in detail the advantages and disadvantages of the procedure and the available options.
•Obtain an informed consent.
Step 6: Prepare for the procedure
•A spinal needle (20G commonly)
•Sterile sheets and instruments
•A manometer
•Antiseptic cleansing agents, Lignocaine 2%
•Numbered collection tubes (at least 4)
•Functioning intravenous access
•Crash cart
•Vital monitoring depending on the patient condition
Step 7: Position the patient
Explain the procedure to the patient if he/she is conscious.
Take informed consent
Lateral recumbent position
•Preferred for an accurate opening pressure.
•Less incidence of post-puncture headache.
•Make the patient acquire a fetal position with the back flexed, to widen the gap between the spinous processes.
•The head flexed, chin close to the chest.
•Hips flexed.
•Knees flexed and as close to the chest as possible.
•Keep the back perpendicular to the bed and close to the edge.
100 Lumbar Puncture |
809 |
|
|
Sitting position
•Lumbar spine should be perpendicular to the bed, leaning forward on a bedside table
•Preferred for obese/elderly/degenerative spine
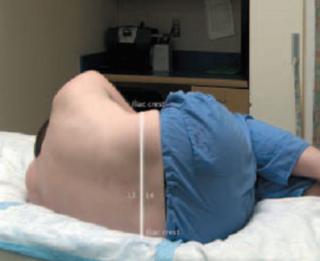
Step 8: Know landmarks and anatomy
Skin-marking pencils should be used to mark before skin preparation:
•Determine the superior point of iliac crests.
•Connect both crests with the imaginary line.
•This line crosses the midline at L4 spine level (spinal cord ends at lower border of L1 in adults).
•Walk the fingers down over the spinous process to palpate L4-L5 and L5-S1 interspaces
•Layers encountered during LP are the following:
–Skin
–Superficial fascia
–Supraspinous ligament
–Interspinous ligament
–Ligamentum flavum
–Epidural space
–Dura
–Arachnoid membrane
Step 9: Procedure
A.Preparation
•Wear the cap, masks, and goggles.
•Scrub appropriately.
•Wear the sterile gown and gloves.
•Prepare the skin:
–Use povidone-iodine or chlorhexidine.
–Cover several interspaces.
•Drape with the sterile fenestrated sheet with the opening over the intended area.
•Cover the iliac crest with the sheet.
B.The procedure
•Apply local anesthesia (2% lignocaine), use a 25-gauge needle, and infiltrate subcutaneously. Use a 20-gauge needle for deeper tissue and aspirate to see that no blood is aspirated before injecting. Inject while withdrawing the needle. Cover a broad area to allow manipulation.
•Systemic sedatives and analgesics can be used under close monitoring.
•Reconfirm the landmarks and interspaces by palpation.
•Insert the spinal needle with stylet in place at superior aspect of inferior spinous process.
•Stay in the midline.
810 |
R. Chawla and C. Gauba |
|
|
•Angle 15–30° cephalad; aim for the umbilicus.
•If the needle is bevel tipped, then keep bevel in sagittal plane. Feel the layers as the needle passes through:
–Popping sensation is felt as the needle passes through the ligamentum flavum.
–Another feeling of giveaway is felt on puncturing the dura.
–Feeling of the layers becomes more consistent with practice.
•Withdraw the stylet to check for flow: if none present, rotate by 90° or advance by 2 mm and recheck.
•If flow is poor, rotate by 90°.
•If bone is encountered, withdraw the needle upto the subcutaneous tissue and redirect the needle superiorly or inferiorly.
•Once the flow is adequate, do the following:
–Measure opening pressure as the height of the fluid via the flexible tube connected to the manometer and needle hub.
–Relax the legs for accurate measurement.
–Measure in recumbent position only (normal pressure 70–180 mm H2O).
–Collect samples and do not aspirate—it may cause hemorrhage.
•Once minimum amount is collected, replace stylet and withdraw the needle.
•Apply pressure at the puncture site, use tincture benzoin to seal, and apply bandage.
•Keep the patient supine for 1–3 h to reduce severity of postdural puncture headache.
Step 10: Know the complications and their management
•Postdural puncture headache
–Most common
–Excessive CSF leak
•Intracranial hypotension
•Stretch on pain-sensitive veins
–Linked to previous history of headaches and psychological factors
–Risk decreased by
•Thinner needles
•Paramedian approach
•Pencil-point needles (controversial)
•Bevel parallel to sagittal dural fibers: to split, not cut
•Replacing the stylet before withdrawing
–Features
•Typically occurs within 72 h and lasts 3–5 days
•Increases on sitting up, better on lying down
•Usually frontal
–Treatment
•Bed rest.
•Hydration.
100 Lumbar Puncture |
811 |
|
|
•Analgesics.
•Methylxanthines—caffeine (most effective), theophylline.
•Epidural blood patch is most effective.
•Epidural injection of saline, dextran, or adrenocorticotropic hormone has been described.
•Hemorrhage (uncommon)
–More risk with bleeding tendency.
–Spinal SAH: radicular pain, paraparesis, sphincter disturbances.
–Spinal subdural hematoma (rare): early surgical intervention, else irreversible neurological damage may occur.
•Difficulty in identifying landmarks or subarachnoid space
–Obesity
–Ankylosing spondylitis
–Kyphoscoliosis
–Lumbar surgery
–Disk degeneration
–Calcification of ligaments
Request for an anesthesiologist or interventional radiologist.
•Dry tap
–The misplaced needle tip
–Dehydration
–Low CSF volume
•Infection (uncommon)
–Seeding of skin flora: preventable by aseptic technique
–More risk with repeated procedures or lumbar drains
•Hemodynamic disturbances
•Cerebral/spinal herniation (see steps 3 and 4)
–Raised ICP
–Cerebrospinal pressure gradient
–Intramedullary/intracerebral mass lesions
•Hearing loss (rare)
–Decreased ICP transmitted to cochlear apparatus
–Reversible
–Underreported
•Sixth nerve palsy
–Reversible
–Traction injury with decreased ICP
•Injury to spinal nerves
–Usually neuropraxia
–Local or referred pain
•Subarachnoid epidermal cysts
–Seeding with skin tissue
–Avoided by a needle with stylet
